|
Low- FODMAP Diet. Jump to Another Topic. Introduction. An Australian research team has developed a new dietary management approach – the Low FODMAP diet – to control symptoms associated with irritable bowel syndrome (IBS). Important to Note – The Diet Requires Expert Guidance. A wide number of health benefits have been attributed to some FODMAPs, which stimulate the growth of beneficial bacteria in the gut. The “Low FODMAP diet” is not a “No FODMAP diet” and it is not a “lifetime diet.”The low FODMAP diet requires the expert guidance of a dietician trained in the area. After 6–8 weeks on the diet, review your progress with the dietician who will advise which foods (and how much) can be gradually re- introduced into your diet. In Australia, the low FODMAP diet is increasingly being accepted as the primary management strategy for IBS, recently adopted by their National Therapeutic Guidelines. IBS affects up to one in seven Americans. It is a condition that is characterized by gut symptoms including abdominal pain, intestinal gas/wind, bloating, and changed bowel habit (ranging from diarrhea to constipation). Symptoms can often be debilitating and lead to a reduced quality of life. A wide range of therapies have been used to control IBS symptoms including various medications, bulking agents and laxatives, and a myriad of lifestyle changes. Most individuals with IBS believe that their symptoms are related to the consumption of certain foods, but advice in this area has been conflicting and confusing and offered little relief for IBS sufferers. Understanding the FODMAP Concept. Carbohydrates can be present in different forms in foods, varying from long- chain carbohydrates (e. Fiber and resistant starch are long- chain carbohydrates resistant to digestion and are important for stool formation and normal bowel function. The Australian group has produced strong evidence that a group of short- chain carbohydrates, named FODMAPs (Fermentable Oligo- saccharides, Di- saccharides, Mono- saccharides And Polyols) are problematic for those with IBS. These short- chain carbohydrates are poorly absorbed in the small intestine and rapidly fermented by bacteria in the gut. The production of gas by these bacteria is a major contributor to symptoms. A pilot study first observed that three out of four patients with IBS responded symptomatically to restriction of FODMAP intake. Subsequently, several high- quality clinical studies have further confirmed that improvement is due to the reduction in FODMAP intake. 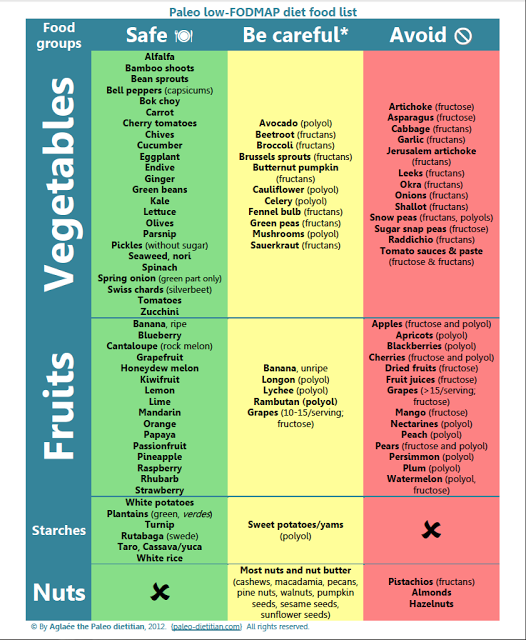
Application of the low FODMAP diet is not only limited to IBS. It has also been shown to improve gut symptoms in more than 5. 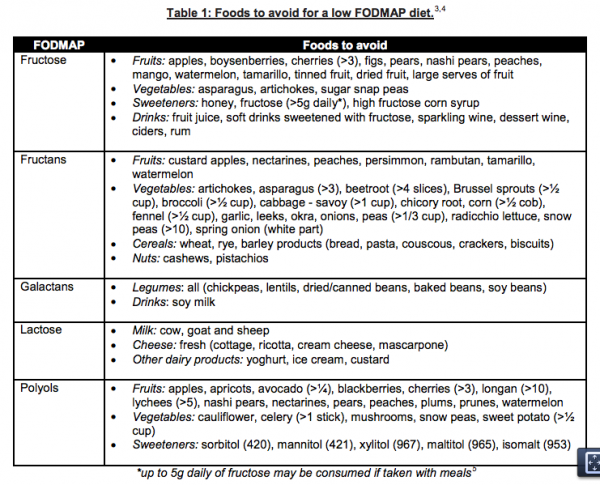 
In patients without a colon, the issue of frequent loose stool production was also reduced significantly. The low FODMAP diet can be tailored to meet an individual’s lifestyle and preferences. Following the low FODMAP approach does not cure IBS, but allows successful drug- free management of symptoms through diet in many patients. Next? Please support IFFGD with a small tax- deductible donation. Adapted from IFFGD Publication #2. CK Yao, Jessica Biesiekierski, Sue Shepherd, Peter Gibson, Eastern Health Clinical School, Monash University, Box Hill Hospital, Melbourne, Australia. 
There are 3 stages to the low FODMAP diet: Stage 1 Restriction: In this stage, you reduce your FODMAP intake by avoiding foods that are high in FODMAPs for 4 to 8.  
I started a low-FODMAP diet but I still experience bloating and diarrhea. If you have fructose malabsorption, elimination of FODMAPs should result in. Low-FODMAP diet suggested foods. Below are low-FODMAP foods categorized by group according to the Monash University "Low FODMAP Diet". Vegetables: alfalfa, bean. 3 Tips for a low FODMAP diet: Follow the diet for 6 weeks. After this, add high FODMAP foods one at a time back into the diet in small amounts to identify foods.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
June 2017
Categories |
 RSS Feed
RSS Feed
